Angioplasty and Stenting: Lifesaving Procedures for Heart Health
Cardiovascular diseases remain the leading cause of mortality globally, necessitating advanced medical interventions to manage and treat conditions like coronary artery disease (CAD). Among the most significant developments in interventional cardiology are angioplasty and stenting. These minimally invasive procedures have revolutionized the treatment of blocked or narrowed arteries, offering patients a way to restore normal blood flow and reduce the risk of heart attacks.
Understanding Coronary Artery Disease
Coronary artery disease is characterized by the buildup of plaque—composed of fat, cholesterol, and other substances—in the coronary arteries, which supply oxygen-rich blood to the heart muscle. This buildup, known as atherosclerosis, narrows the arteries and reduces blood flow, leading to chest pain (angina), shortness of breath, and other symptoms. In severe cases, a complete blockage can cause a heart attack.
What is Angioplasty?
Angioplasty, also known as percutaneous coronary intervention (PCI) or percutaneous transluminal coronary angioplasty (PTCA), is a procedure designed to open clogged heart arteries. It involves the use of a balloon catheter, which is inserted into the narrowed artery and then inflated to widen the vessel, allowing for improved blood flow.
Steps of the Angioplasty Procedure:
Preparation: The patient is given a local anesthetic and, in some cases, mild sedation. A sheath is inserted into an artery in the groin, wrist, or arm.
Catheter Insertion: A thin, flexible tube called a catheter is threaded through the sheath and guided to the coronary artery using X-ray imaging.
Balloon Inflation: A second catheter with a small balloon at its tip is advanced through the first catheter to the site of the blockage. The balloon is then inflated, compressing the plaque against the artery walls and widening the artery.
Restoring Blood Flow: The balloon is deflated and removed, leaving the artery wider and enhancing blood flow to the heart muscle.
What is Stenting?
Stenting often accompanies angioplasty to ensure that the artery remains open. A stent is a small, mesh-like tube that acts as a scaffold to support the arterial walls and prevent them from collapsing or becoming re-narrowed.
Types of Stents:
Bare-Metal Stents (BMS): These stents are made of stainless steel or cobalt-chromium alloy and do not contain any coatings. They provide immediate support to the artery but have a higher risk of restenosis (re-narrowing of the artery).
Drug-Eluting Stents (DES): These stents are coated with medication that is gradually released to prevent scar tissue from forming within the artery, significantly reducing the risk of restenosis. Common drugs used include sirolimus, paclitaxel, everolimus, and zotarolimus.
Bioresorbable Vascular Scaffolds (BVS): These are newer, temporary stents made from materials that dissolve over time, leaving the artery free of any permanent foreign objects.
The Procedure of Stenting:
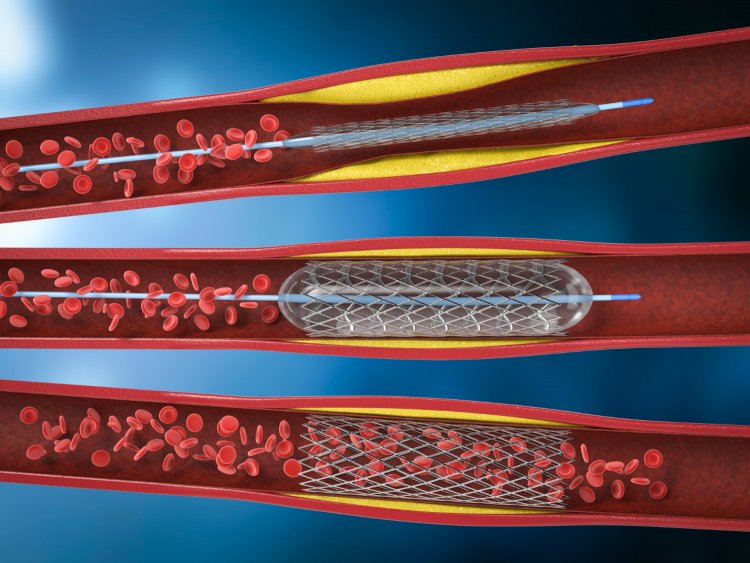
Placement: After balloon angioplasty, the stent, mounted on a balloon catheter, is positioned at the blockage site.
Expansion: The balloon is inflated, expanding the stent and pressing it against the artery walls.
Final Positioning: The balloon is deflated and removed, leaving the stent permanently in place to keep the artery open.
Post-Deployment: In some cases, a second balloon may be used to further expand the stent and ensure it is firmly in place.
Indications for Angioplasty and Stenting
Angioplasty and stenting are recommended for patients with:
- Stable Angina: Chest pain that occurs during physical activity or stress.
- Unstable Angina: Sudden, severe chest pain that occurs at rest or with minimal exertion.
- Acute Myocardial Infarction (Heart Attack): Immediate intervention to restore blood flow to the heart muscle.
- High-Risk Stress Test Results: Indicating significant blockage that may lead to a heart attack.
- Failed Medical Therapy: When medications and lifestyle changes are insufficient to manage symptoms.
Benefits of Angioplasty and Stenting
Angioplasty and stenting offer several advantages over traditional open-heart surgery:
- Minimally Invasive: These procedures involve small incisions, reducing recovery time and the risk of complications.
- Shorter Hospital Stay: Patients typically spend only one to two days in the hospital, compared to a week or more for open-heart surgery.
- Quick Recovery: Most patients return to their normal activities within a week.
- Reduced Symptoms: These procedures effectively relieve symptoms of chest pain (angina) and shortness of breath.
- Reduced Risk of Heart Attack: By restoring blood flow, these procedures decrease the likelihood of a future heart attack.
Risks and Complications
While generally safe, angioplasty and stenting carry some risks, including:
- Restenosis: Despite advancements, there is still a risk of the artery re-narrowing, particularly with bare-metal stents.
- Blood Clots: Stents can sometimes promote clot formation, which can lead to a heart attack. Patients are usually prescribed blood-thinning medications to mitigate this risk.
- Bleeding: The catheter insertion site can bleed or become infected.
- Artery Damage: Rarely, the artery can be damaged during the procedure.
- Allergic Reactions: To the contrast dye used during the procedure.
- Kidney Damage: From the contrast dye, especially in patients with pre-existing kidney issues.
Advances in Angioplasty and Stenting
Recent technological advancements have further improved the outcomes of these procedures:
- Optical Coherence Tomography (OCT) and Intravascular Ultrasound (IVUS): Provide detailed images of the inside of the arteries, helping cardiologists to accurately place stents and assess the results.
- Fractional Flow Reserve (FFR): Measures pressure differences across a coronary artery stenosis to determine the likelihood of improved blood flow after angioplasty.
- Biodegradable Stents: Newer stents that dissolve over time, reducing long-term complications.
Post-Procedure Care
After undergoing angioplasty and stenting, patients are advised to follow a strict regimen to ensure long-term success:
- Medications: Continuing prescribed medications, such as antiplatelet agents (e.g., aspirin and clopidogrel), is crucial to prevent clotting.
- Lifestyle Changes: Adopting a heart-healthy lifestyle, including a balanced diet, regular exercise, smoking cessation, and stress management, is vital.
- Regular Check-ups: Routine follow-up appointments with a cardiologist help monitor heart health and detect any issues early.
- Cardiac Rehabilitation: A structured program of exercise and education to help patients recover and reduce the risk of future heart problems.
Angioplasty and stenting have transformed the landscape of cardiovascular care, offering effective solutions for patients with coronary artery disease. These procedures not only improve the quality of life by alleviating symptoms but also play a critical role in preventing severe cardiac events like heart attacks. As medical technology continues to advance, the efficacy and safety of angioplasty and stenting are expected to further improve, providing hope and relief to millions of heart patients worldwide.
Disclaimer: The information provided in this article is for educational purposes only and should not be considered medical advice. If you have any health concerns or are experiencing symptoms, it is important to consult with a healthcare professional, such as a doctor or clinic, for proper diagnosis and treatment. Always seek the advice of your doctor or other qualified health provider with any questions you may have regarding a medical condition. Do not disregard professional medical advice or delay in seeking it because of something you have read in this article.
#healthcare #angioplasty #stenting #hearthealth #cardiology #medicalprocedures #heartdisease #medicaladvancements #healthtips #cardiaccare
What's Your Reaction?





















